Do flip flops cause foot and toe pain? Read what to look for in a summer sandal and tips for flip flop lovers written by top foot and ankle experts!
CONTINUE READING →The Link Between Foot Health and Posture
Common foot conditions can lead to discomfort in various body parts. How do these conditions influence posture?
CONTINUE READING →Why Are My Feet Different Sizes? It’s More Common Than You Think
Why do my feet differ in size? Discovering the reasons behind differing foot sizes can help alleviate discomfort and ensure proper foot care.
CONTINUE READING →Custom Orthotics vs. Over-the-Counter Inserts: Which Are Best for Your Feet?
Custom Orthotics vs. Over-the-Counter Inserts: Are store-bought inserts sufficient for foot health, or do custom orthotics offer superior support and relief?
CONTINUE READING →Revealing the Secrets of Men’s and Women’s Shoe Sizes: Why Are They Different?
Why are men's and women's shoe sizes different? Are there actually differences between women's and men's shoes and feet?
CONTINUE READING →9 Running Tips from Sports Medicine Experts
Whether you’re a beginner runner, an experienced runner looking to improve, or returning to running after some time away, there’s always something to learn!
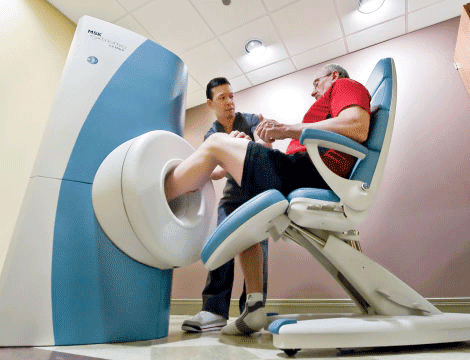
CONTINUE READING →Revolutionizing Extremity Imaging: UFAI’s Open MRI for the Foot and Ankle
We are excited to offer the ONI MSK open scanner - designed for imaging of extremities and only the joint being imaged is inside the scanner.
CONTINUE READING →Common Foot Problems In Aging Feet: What To Watch Out For
Aging feet need special care as the risks for chronic foot problems increase. Learn more about common foot problems to watch for as we age.
CONTINUE READING →How to Choose Running Shoes: 6 Essential Steps
What's the best running shoe for your foot type? Los Angeles foot specialists discuss the best options for overpronation, underpronation, and normal arched feet.
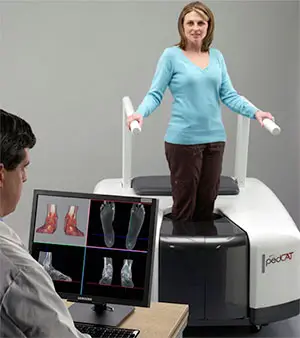
CONTINUE READING →State-of-the-Art CT Scanning, Now in Our Office
UFAI, the only location in Southern California with the pedCAT foot and ankle cone-beam CT scanner. The first true weight bearing imaging machine.
CONTINUE READING →The Power of Pediatric Flexible Flatfoot Procedures
Does pediatric flatfoot require surgery? Our expert podiatrist discusses treatment options for pediatric flatfoot.
CONTINUE READING →If the Shoe Fits, Wear it… Especially for Kids Shoes!
Many adult foot problems can be traced back to ill-fitting shoes forced onto young feet. Read what our experts say about fitting your kids' shoes.
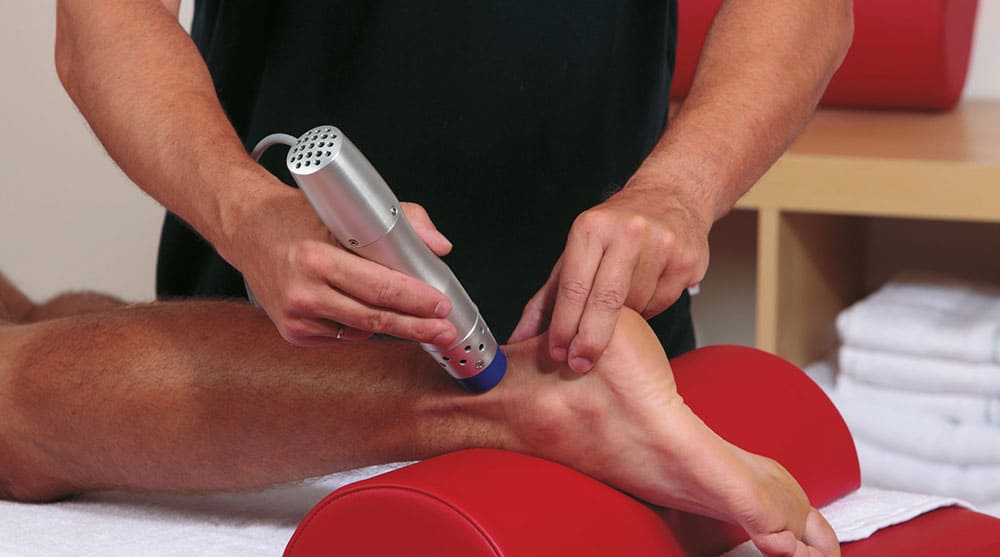
CONTINUE READING →An Inside Look at Shockwave Therapy for Heel Pain, now available in Valencia, CA
State-of-the-art shockwave therapy for heel pain is now available in Valencia. UFAI offers pain free therapy for plantar fasciitis and other causes of pain.
CONTINUE READING →StimRouter: A Revolutionary Approach to Targeted Pain Relief
University Foot and Ankle Institute is excited to offer our patients an innovative solution for targeted pain relief: the StimRouter by Bioventus. Many of my patients have expressed concerns about managing chronic pain, and the StimRouter is a game-changing device that addresses these concerns. This innovative medical device’s targeted approach to pain relief provides an excellent option for those struggling read more »
CONTINUE READING →Is Barefoot Running Better? Or are you Running Toward Injury?
Patients often ask if barefoot running is safe. There are many factors to consider before making the switch to barefoot running.
CONTINUE READING →15 Summer Foot Care Tips to Put Your Best Feet Forward
A healthy foot is an attractive foot! Here are 15 tips for better foot health in the summer months.
CONTINUE READING →Lawn Mowing Causes Lots of Foot Injuries: How to Stay Safe!
Lawn mowing safety is important! Mowers cause thousands of injuries every year — about 20% are foot injuries. Top tips to protect you (and your kids!)
CONTINUE READING →What is Synovial Sarcoma? A Rare and Dangerous Cancer
Sarcomas are cancerous tumors that grow in muscles, fat, joints, nerves, or blood vessels. Though they are rare, they can be very serious and should be treated immediately.
CONTINUE READING →Surgical Site Infections: What You Need To Know
What is a surgical site infection? A surgical site infection (SSI) is a severe complication following a surgical procedure; as the name implies, it is an infection at the site of surgery. At the University Foot and Ankle Institute (UFAI), our podiatrists are vigilant regarding foot and ankle surgery postoperative care and infection control. While an infected surgical wound may read more »
CONTINUE READING →Avoiding Foot and Ankle Overuse Injuries While Dog Walking
We often see a rise in foot and ankle injuries once summer comes. More walking dogs means more walking and more overuse injuries.
CONTINUE READING →