- Home
- Foot & Ankle Conditions
- Diabetic Foot Conditions
Diabetic Foot Conditions
Why do diabetics have foot problems?
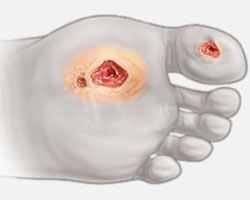
For diabetics, ordinary foot problems can quickly lead to infection and serious complications.
High blood sugar caused by poorly controlled diabetes can cause nerve damage (neuropathy) —especially to nerve cells in the feet. When nerves are damaged, they don’t accurately report pain to the brain.
Pain is our body's alarm system, letting us know that something needs attention. Without this vital sensory feedback, you might overlook a minor injury like a cut, blister, or sore. If left untreated, these small problems can become serious.
-
Foot and Ankle Surgeon and Director of University Foot and Ankle Institute
Dr. Bob Baravaria DPM, FACFAS is a Board-Certified Podiatric Foot and Ankle Specialist. He is an assistant clinical professor at the UCLA School of Medicine and serves as Director of University Foot and Ankle Institute.
Dr. Baravarian has been involved in athletics his entire life and played competitive tennis in high school and college. He has an interest in sports medicine, arthritis therapy, and trauma/reconstructive surgery of the foot and ankle. He is also fluent in five languages (English, French, Spanish, Farsi, and Hebrew),
Diabetic foot condition articles from our blog
- Common Foot Problems In Aging Feet: What To Watch Out For
- Neuropathy and Nerve Compression: Causes, Symptoms and Treatment
- Diabetic Foot Conditions: Charcot Foot
- Diabetic Foot Conditions: Osteomyelitis
- Why Diabetic Foot Exams Are Critically Important
- Do Your Burning Feet or Numb Toes Need to See a Doctor? Here's How to Know
- 6 Beach Bummers for Your Feet
 You guys are the best, I don’t know what I would do without Dr.Franson, Suzanne and Jen.Suzanne N.
You guys are the best, I don’t know what I would do without Dr.Franson, Suzanne and Jen.Suzanne N. Great experience. Great communication. Great direction for my care. Very happy I chose to go with this particular doctor and o...Christopher R.
Great experience. Great communication. Great direction for my care. Very happy I chose to go with this particular doctor and o...Christopher R. Great service and care. Highly recommend Dr. Franson.David B.
Great service and care. Highly recommend Dr. Franson.David B. If you have to go see a Doctor than this is a great experience.Frank M.
If you have to go see a Doctor than this is a great experience.Frank M. My doctor was great. Really greatRudolph B.
My doctor was great. Really greatRudolph B. Good.David E.
Good.David E. Great office and great care. Dr. Redkar has been excellent overseeing the healing process. Hoping surgery will not be necessary...Christopher C.
Great office and great care. Dr. Redkar has been excellent overseeing the healing process. Hoping surgery will not be necessary...Christopher C. Your Santa Barbara office and Dr. Johnson always give me excellent care!Jayne A.
Your Santa Barbara office and Dr. Johnson always give me excellent care!Jayne A. Dr. Gina Nalbadian was amazing!! I came in with an emergency foot situation and she had wonderful bedside manner and resolved m...Danielle C.
Dr. Gina Nalbadian was amazing!! I came in with an emergency foot situation and she had wonderful bedside manner and resolved m...Danielle C. I was frustrated that after 3 weeks I still hadn’t heard back about my PT referral status. And I did sit in a room for over 30 ...Sarah C.
I was frustrated that after 3 weeks I still hadn’t heard back about my PT referral status. And I did sit in a room for over 30 ...Sarah C. Amazing Doctor Dr Babak just did my bunion surgery fealt amazing after This is one of the best foot Surgeon i highly recommend ...Nathalie D.
Amazing Doctor Dr Babak just did my bunion surgery fealt amazing after This is one of the best foot Surgeon i highly recommend ...Nathalie D. I’m very pleased with Dr. Kelman.Alan S.
I’m very pleased with Dr. Kelman.Alan S.
-
 Listen Now
Do Your Burning Feet or Numb Toes Need to See a Doctor? Here's How to Know
Read More
Listen Now
Do Your Burning Feet or Numb Toes Need to See a Doctor? Here's How to Know
Read More
-
 Listen Now
Diabetic Foot Conditions: Charcot Foot
Read More
Listen Now
Diabetic Foot Conditions: Charcot Foot
Read More
-
 Listen Now
Diabetic Foot Conditions: Osteomyelitis
Read More
Listen Now
Diabetic Foot Conditions: Osteomyelitis
Read More
-
 Listen Now
Common Foot Problems In Aging Feet: What To Watch Out For
Read More
Listen Now
Common Foot Problems In Aging Feet: What To Watch Out For
Read More
-
 Listen Now
Neuropathy and Nerve Compression: Causes, Symptoms and Treatment
Read More
Listen Now
Neuropathy and Nerve Compression: Causes, Symptoms and Treatment
Read More
-
 Listen Now
Why Diabetic Foot Exams Are Critically Important
Read More
Listen Now
Why Diabetic Foot Exams Are Critically Important
Read More
-
 Listen Now
6 Beach Bummers for Your Feet
Read More
Listen Now
6 Beach Bummers for Your Feet
Read More