- Home
- UFAI in the News
- UFAI Medical Journals
- Correction of Hallux Abducto Valgus
Correction of Hallux Abducto Valgus
- Published 4/18/2014
- Last Reviewed 4/18/2014

Written by Dr. L. Mae Chandler, DPM
An array of distal first metatarsal osteotomies has been described over the decades for the correction of hallux valgus. No one procedure is proficient in correcting all forms and severities of hallux valgus deformities. To optimize results, it is imperative for the surgeon to match a procedure and its modifications to the patient’s deformity. The dorsal long arm chevron osteotomy stands at the forefront for correction of mild to moderate hallux abductovalgus. The results with this specific osteotomy are predictable; it allows for early ambulation, and it is easily modified to compensate for the deformity at hand.
Introduction
There have been numerous procedures described over the years for the correction of hallux abducto valgus deformities. These procedures vary from simple “bumpectomies” to first metatarsal head osteotomies to more involved basilar osteotomies and even corrective arthrodesis. Secondary to early weight-bearing, the ability to tackle deformities in multiple planes, and technical ease, the distal metatarsal osteotomies have persevered as the most popular form of correction for mild to moderate deformities. One of the most debated complications of distal metatarsal osteotomies is that of avascular necrosis (AVN). Literature supports both the prevalence of avascular necrosis following the distal metatarsal osteotomy and the lack thereof. Another complication that can cause less than desirable results is first metatarsophalangeal joint (MTPJ) stiffness.
Surgical treatment decision-making
There have been over 300 surgical procedures described in the literature for the correction of hallux valgus deformity. It is imperative to remember that not one procedure is sufficient to correct all bunion deformities. The decision-making process must commence with the understanding that not all hallux valgus deformities are equal. When evaluating a deformity, there are many factors that must be considered. These factors include the patient’s chief complaint, occupation, age, expectations, and athletic interests. Thorough physical examination of the patient’s lower extremity and radiograph evaluation consisting of weight-bearing foot films are also essential in the decision-making process.
The theory that reduction of an abnormal first intermetatarsal (IM) angle is essential to hallux valgus repair is well established. A variety of bony procedures are used for correction of metatarsus primus varus. These osteotomies are located at the distal portion of the metatarsal (head and neck), the midshaft and the base of the metatarsal, and corrective arthrodesis of the first metatarsocuneiform joint. Many algorithms have been developed to provide physicians with a logical scheme with which to approach a patient with a hallux valgus deformity.
Distal metatarsal osteotomies are indicated for mild to moderate hallux valgus deformities. These procedures are intended for structural correction of the deformities of hallux abducto valgus manifested at the level of the first metatarsal head, such as increased IM angle, frontal plane rotation of the first metatarsal head, sagittal plant deformity of the first metatarsal head, and increased proximal articular set angle (PASA). Radiographically the hallux valgus angle (HVA) is less than 40°, the IM angle is less than 20°, and a there is subluxation of the first MTPJ.
Because of several advantages, including relative ease of performance, metaphyseal location, and mechanically stable geometry, the chevron osteotomy has gained significant popularity.1 The combination of these features facilitates rapid osseous union and early weight-bearing. Midshaft and basilar osteotomies are characteristically indicated because the IM angle exceeds 15 to 20°. Commonly these osteotomies are accompanied by diminished intrinsic stability despite fixation, thus requiring periods of non-weight-bearing and immobilization.
Historical review
Reverdin
Reverdin2 was the first to describe correction of hallux valgus deformity by means of a distal first metatarsal osteotomy in 1881. This procedure required a medially based wedge osteotomy in the frontal plane preserving the lateral cortex. The osteotomy is located proximal to the articular surface of the metatarsal head and distal to the sesamoid apparatus. The original intention was correction of an abnormal proximal articular set angle (PASA). This osteotomy was linked with difficult fixation and potential sesamoid disturbance.
Green3 then described a modification to the Reverdin procedure in 1977, changing the osteotomy design to a horizontal L to evade possible damage to the dorsal articular surface of the sesamoids or the sesamoidal grooves beneath the metatarsal head. In this modification, the lateral hinge remained intact and therefore did not attend to the IM angle or sagittal plane deformities.
In 1988, Laird and coworkers4 published another modification to the Reverdin using Green’s modification as well as completing the vertical osteotomy cut by passing through the lateral cortex of the first metatarsal head and resecting a medially based wedge of bone from the plantar shaft of the metatarsal. By transposing the distal part of the first metatarsal head laterally, this modification affords a relative reduction of the metatarsus primus adductus angle as well as reducing the proximal articular set angle (PASA). The medially based wedge of bone resected would also reduce any valgus rotation of the great toe.
A year later, Zyzda and Hineser used a bone graft to alleviate possible shortening as well as to correct sagittal plane deformity. They advised rotating the resected dorsal wedge of bone 180° and reinserting it into the dorsal osteotomy site with the base adjusted laterally as an autogenous bone graft to compensate for a sizable proximal articular set angle (PASA) or short first metatarsal. Likewise, the resected wedge was inserted into the plantar osteotomy with the base of the wedge lateral to account for a valgus deformity or the graft could be inserted to plantarflex the metatarsal head. These authors thought this technique avoided excessive correction and therefore overcorrection.
Today, the Reverdin is often added as an adjunct procedure to basilar osteotomies or arthrodesis to primarily account for a large PASA, most likely caused by the osteotomy’s innate lack of fixation options. Lombardi and colleagues6 described adding the Reverdin to a Lapidus procedure if soft tissue correction of the valgus deformity is deficient or the PASA is exceptionally large. However, with this combined approach considerable shortening of the first metatarsal occurs, yet Lombardi found no occurrence of lesser metatarsalgia complaints, which he attributed to sufficient plantarflexion of the metatarsal at the arthrodesis site.
Hohmann
The first surgeon accredited with describing a procedure that concurrently tackled abnormalities involving the metatarsus primus adductus angle, metatarsus primus elevatus, and the proximal articular set angle (PASA) was Hohmann. His operative technique used a complete trapezoidal osteotomy located at the anatomic neck of the first metatarsal with the widest part located medially. The location at the metatarsal neck avoided the sesamoid apparatus, decreasing the prospect of developing sesamoid arthritis. Hohmann did not believe in transecting the medial eminence; therefore, the whole procedure was performed extracapsularly. This procedure is referenced purely for a historical reference. It is no longer performed as originally depicted secondary to its unstable osteotomy and high frequency for dislocation.
Many modifications to the Hohmann procedure were fashioned to bestow more stability to the osteotomy site as well as resect the medial eminence while still attempting the same end result. In 1984, Warrick and Edelman7 examined certain modifications such as resection of the medial eminence and altering the direction of the wedge resection to an oblique orientation rather than transverse, which permitted proper screw fixation. This modified Hohmann bunionectomy was performed on 15 feet in 11 patients. The average preoperative first IM angle was 12.5° with a postoperative angle of 7.7°. The width of the first metatarsal shaft was a limiting factor as well as the shortening that subsequently occurred when increasing the obliquity of the osteotomy to correct a greater IM angle. The amount of PASA correction was established by the size of the trapezoidal wedge resection. The authors uncovered, on average, a 4.1-mm shortening of the first metatarsal that they thought to be the most disadvantageous complication to this modified Hohmann procedure. Thus, the application of this procedure has been limited to mild to moderate hallux valgus deformities.
Mitchell
In 1945, Hawkins and colleagues8 described a transpositional, step-cut osteotomy to correct the IM angle combined with resection of the medial eminence. It was Mitchell who later described and popularized a biplanar metaphyseal osteotomy, which displaced the capital fragment both laterally and plantarly, also shortening the first metatarsal. Merkel and colleagues9 performed a retrospective study of 96 Mitchell first metatarsal osteotomies with an average follow-up of 7 years. Only 59% of those patients were available for follow-up. They found excessive first metatarsal shortening, dorsiflexion of the osteotomy, and failure to correct the first IM angle to 10° or less were all associated with overall patient dissatisfaction. Shortening of the first metatarsal was found to be more than 5 mm in 39 of the 56 patients available for follow-up.
The removal of a rectangular wedge of bone while attempting to retain a lateral cortical spike produces a technically demanding procedure. Significant shortening results from wedge removal that subsequently may generate lesser metatarsalgia. The threat of enhanced angulation and displacement are also probably secondary to the inherent instability of the osteotomy. Therefore, patients undergoing this procedure must be non-weight-bearing for a period of time even though most patients are able to bear weight right away following most distal metatarsal osteotomies.
Wilson
In 1963, Wilson described a through-and-through osteotomy oriented 45° from the transverse plane. This osteotomy began medially at the proximal aspect of the medial eminence and coursed in a distal-medial to proximal-lateral direction attending to the IM angle and PASA. Several complications proceeded this procedure, including shortening, inherent instability, dorsiflexion, lesser metatarsalgia, and recurrence to name a few.
Many modifications to the Wilson osteotomy ensued. Helal and colleagues described orienting the osteotomy 45° to the sagittal plane, preventing dorsiflexion as well as plantarflexion of the capital fragment to compensate for any shortening. Grace and colleagues reinforced the medial capsule by suturing a medial flap of capsule under tension to the periosteum or through a drill hole in the metatarsal shaft. Allen and colleagues were the first to use internal fixation by placing a screw, which permitted simultaneous correction of an increased IM angle and a laterally deviated cartilaginous surface.
DRATO
Johnson and Smith13 first described the DRATO procedure, a derotational, angulation, transpositional osteotomy of the first metatarsal head. The preoperative criteria include frontal plane rotational of the metatarsal head, abnormal proximal articular set angle (PASA), plantarward adaptation of the articular surface of the first metatarsal, mild increase of the IM angle, and a normal distal articular set angle. Because the preoperative criteria for this procedure are so specific, very few cases tend to be performed.
Chevron
In 1962, Austin first performed a horizontally directed “V” displacement osteotomy for the correction of hallux valgus. However it was not until 1981 that Austin and Leventen1 published their description of a distal chevron osteotomy of the first metatarsal. In this publication, they reviewed more than 1200 patients in which the chevron osteotomy was performed. Their objective was to construct a procedure that addressed 3 key points: restoring the alignment of the first MTPJ, correcting the hallux valgus, and correcting the metatarsus primus varus while maintaining osteotomy stability and allowing early ambulation.
Originally this osteotomy did not include fixation. Austin thought the shape of the osteotomy as well as the impaction of the cancellous capital fragment on the shaft of the first metatarsal offered ample stability to sacrifice fixation. In 1985, Jahss and colleagues assessed the operative effectiveness of 5 distinct metatarsal osteotomies for hallux valgus correction. The series had 120 feet evaluated via radiography over a 5-year period and the osteotomies included biplanar neck, chevron, biplanar basilar, basilar concentric, and basilar concentric with a lateral closing wedge. All the osteotomies with the exception of the chevron had varying plantar displacement of the capital fragment and fixation with crossed K-wires. They found the chevron gave the least amount of correction by approximately 2° and there was a 12.5% loss of correction secondary to the absence of fixation. Hattrup and Johnson interviewed 154 patients with 225 chevron osteotomies: 79.1% of the procedures conveyed complete satisfaction, 12.9% stated satisfaction with minor reservations, and 8% were dissatisfied. Failure to achieve correction and technical errors were the major factors generating incomplete satisfaction.
Several modifications in the technical part of the procedure have been made since the initial depiction. These modifications have included the use of various alternative methods of internal fixation, altering the angle of the osteotomy, and augmenting with additional procedures. Numerous modifications have been created as surgeons try to benefit from the advantages of these procedures while addressing their deficiencies.
Kalish
Possibly the most popular modification to the Austin osteotomy is that of the Kalish or long dorsal arm, which is more amendable to screw fixation. This modification was fashioned to address the limitations of the standard Austin procedure, including displacement and malposition of the capital fragment, delayed or nonunion, difficulties with fixation, and limited postoperative first MTPJ range of motion. The dorsal long arm osteotomy allowed for correction of larger deformities by permitting greater lateral displacement of the capital fragment. Also, 2-screw fixation was feasible, which has been found to distribute the compression forces across the osteotomy more evenly and resists rotation of the capital fragment.
Youngswick
In 1982, Youngswick described a modification to the chevron osteotomy that would also plantarflex the metatarsal head for a reduction of metatarsus primus elevatus while maintaining the 60° horizontal “V” osteotomy. This modification was achieved by placing a second osteotomy parallel to the original dorsal osteotomy from the classic chevron osteotomy. This second osteotomy therefore permitted a preset portion of bone to be removed so that after impaction of the capital fragment on the metatarsal shaft, plantarflexion of the metatarsal head ensued. A true biplanar correction results when combining this modification with the lateral displacement of the classic chevron osteotomy.
Percutaneous Technique
Bösch and colleagues first described a percutaneous transverse distal metatarsal osteotomy in 2000 and Giannini and colleagues in 2003 and Magnan and colleagues in 2005 further popularized the technique. Current trends for surgical treatment are toward minimally invasive procedures that entail minimal soft tissue stripping, theoretically decreasing morbidity. The percutaneous procedure described by Giannini and colleagues begins with a 1-cm medial incision at the first metatarsal neck directly down to bone.A complete osteotomy is performed at the metatarsal neck by using an oscillating bone saw. The capital fragment is displaced to correct the hallux valgus angle (HVA), intermetatarsal angle (IMA), and distal metatarsal articular angle (DMAA) and is stabilized with a 2-mm K-wire. Their results showed no avascular necrosis of the first metatarsal head nor pseudoarthrosis of the osteotomy. The mean preoperative HVA was 33; mean preoperative IMA was 13, and the mean preoperative DMAA was 20. At an average follow-up of 7 years, the HVA was 16; IMA was 7, and the DMAA was 8.
As the distal first metatarsal osteotomies have evolved, so too have the fixation options. They comprise impaction (which in theory is not a fixation method), sutures, Kirschner wires, metallic screws, staples, absorbable screws, nonlocking plates, and locking plates. Metallic screws tend to be the most fashionable method of fixation of a distal metatarsal osteotomy. Screw fixation provides relative stability as well as compression, when inserted via a lag technique. Rotational stability may also be achieved if 2 screws are placed across the osteotomy.
Operative technique
Anesthesia is usually obtained with local anesthesia and intravenous sedation. An ankle pneumatic tourniquet is applied and inflated to 250 mm Hg to achieve the desired hemostasis. The incision is placed medially near the junction of the plantar and dorsal skin. This technique tends to produce a nicer cosmetic result than that of a dorsal or dorsal-medial incision. The incision is deepened by blunt dissection, taking care to retract neurovascular structures and cauterize superficial veins. A plane is created between the capsule of the first MTPJ and the subcutaneous tissue, which allows retraction of the subcutaneous tissue and its neurovascular elements as one unit. The capsulotomy is then performed using a semi-elliptical incision at the dorsomedial shoulder of the first metatarsal head and subsequently the redundant capsule is removed.
The medial eminence is resected parallel with the medial border of the foot by using an oscillating saw. The specific osteotomy is chosen and carried out in the metaphyseal region to provide a larger surface area for bone contact. The authors prefer a long dorsal arm chevron osteotomy, allowing for a 2-screw fixation, which has been found to be quite stable and decreases rotational forces.
The metaphyseal bone aids in rapid healing and is relatively stable for fixation. In 1997, Badway and colleagues reported that capital fragment following a chevron osteotomy could be displaced laterally up to 6 mm in male and 5 mm in female patients, which represents approximately 30% displacement of the metatarsal’s width. However, some have advocated translating the capital fragment greater than 30% to expand the indications for the chevron osteotomy to include first IM angles in excess of 20°. In a retrospective study by Stienstra and colleagues 38 bunionectomy cases with large displacement distal chevron osteotomies (greater than or equal to 40% lateral translation) were found to have an average lateral translation of 9.8 mm with a relative change of the IM angle of 10°.
A 1.5 cm × 1.5 cm amniotic membrane graft is then placed on the dorsal aspect of the first metatarsal head and the capsule is closed with 2.0 Vicryl. Subcutaneous tissue is closed with 4.0 Monocryl and the skin is reapproximated with 5.0 nylon. Sterile compressive dressing is applied consisting of Xeroform, 4 × 4 gauze, Webril, Kling, and Coban. The tourniquet is released and the short Cam walker boot is applied while patient is still on the operating table.
Postoperative management
The patient is placed into a short Cam walker boot and is instructed to be weight-bearing as tolerated in the boot at all times. The patient’s first postoperative appointment in the office is 5 days after surgery. The Cam walker boot is removed at this time and radiographs are taken in the office, including 3 views weight-bearing of the surgical foot. The bandage is changed and a fresh bandage is applied as well as the Cam walker boot. The patient is instructed to continue to weight-bear as tolerated in the boot. At 2 weeks after surgery, skin sutures are removed, allowing the patient to get incision site wet now and begin passive range-of-motion exercises about the first MTPJ. The patient continues in the short Cam walker boot for an additional 2 weeks. Radiographs are obtained again at 4 weeks after surgery, and if osseous healing is satisfactory, the patient is transitioned into a stiff-soled shoe and physical therapy may be initiated to increase the first MTPJ range of motion. Approximately 6 weeks after surgery, the patient may begin to increase activity as tolerated.
Complications
Just as any other surgical procedure, first metatarsal head osteotomies also have their share of possible complications. These complications can range from chronic edema to avascular necrosis of the first metatarsal head. The more common complications include delayed union, limited first MTPJ motion, lack of toe purchase, chronic edema, hallux varus/adductus, and hallux abductus. Less common complications, such as intraoperative fracture, excessive shortening, elevatus of the first metatarsal head, and avascular necrosis, may have decreased in prevalence secondary to better preoperative criteria and improved surgical instrumentation.
A common complaint after distal metatarsal osteotomies intended to treat hallux valgus is decreased first MTPJ range of motion. Jones and colleagues found limited joint motion in approximately 8% of patients following head osteotomies in their retrospective statistical analysis of complications after hallux abducto valgus surgery. The authors thought the limited range of motion was secondary to first metatarsal elevates and to intracapsular adhesion.
Transfer metatarsalgia may occur secondary to excessive shortening of the first metatarsal, which in turn increases the pressure borne by the second metatarsal. Jahss and colleagues state that second metatarsalgia, commonly present in conjunction with a hallux abducto valgus deformity, is further provoked by surgical procedures that shorten the first metatarsal, dorsally tilt the capital fragment, or cause loss of hallux purchase. Shapiro and Heller noted 33% of patients reported lesser metatarsalgia following a Mitchell osteotomy. Because an innate part of the Mitchell osteotomy is shortening, the authors thought the Mitchell procedure was not indicated for patients whose first metatarsal was more than 4 or 5 m shorter than the second preoperatively. Conversely, Merkel and colleagues9 found in their series of 96 Mitchell osteotomies that the primary cause of transfer metatarsalgia was dorsal displacement of the capital fragment. It is vital that the capital fragment is plantarflexed to prevent this complication.
It is essential to consider both the functional and the structural deformities of hallux valgus. When the deformity is treated surgically as only a functional or structural deformity, troubles will occur in overcorrection and undercorrection. Undercorrection or recurrence of hallux valgus is often secondary to insufficient soft tissue release or poor structural correction. The metatarsus adductus angle and the first metatarsal width are key factors when preoperatively evaluating the parameters, which will aid in the selection of the proper procedure.
It has been recorded in the literature that recurrence of hallux valgus deformity occurs in approximately 10% of cases. It is thought that this recurrence rate could be significantly lessened if the indications for the procedure are not overextended. Hattrup and Johnson reported recurrence of the deformity in 18 of 225 procedures, whereby the average preoperative hallux abductus angle of 37° was corrected to an average of 31° postoperatively. Hirvensalo and colleagues noted in 78 chevron ostetotomies that were performed in 60 patients with painful hallux valgus, and a recurrence of the deformity occurred in 8 feet (10%). They found that hallux valgus recurred when the preoperative hallux abductus angle averaged 37° or more and the first IM angle averaged 13° or more. The risks of recurrence, undercorrection, and/or malunion are increased when using distal metatarsal osteotomies for more severe deformities.
Possibly the most severe complication is AVN. The incidence of AVN has been reported as low as 0% and as high as 20% following a distal chevron osteotomy. Jones and colleagues explored the blood supply to the first metatarsal head in a cadaveric study. Using latex injection and a modified Spalteholz technique, they discovered an extraosseous network of vasculature proximal and distal to the chevron osteotomy. When the osteotomy is performed properly, both networks were preserved. Potential technical errors, such as overpenetrating the saw blade and erroneous placement of the proximal arms of the osteotomy inside the joint capsule, could cause severing of the dorsal metatarsal artery.
The use of an amniotic membrane to augment distal metatarsal osteotomies in hallux abducto valgus surgery
The amniotic membrane is a new allograft that is procured from electively donated placentas after childbirth. This placental tissue bears unique biologic properties that promote regenerative healing while controlling inflammation and preventing scar. This bioactive matrix encloses exclusive matrix proteins that regulate inflammation and prevent scar formation, which could further lead to limited functional recovery, poor cosmesis, and further surgery.
One potentially devastating complication after first metatarsal head osteotomies is first metatarsophalangeal joint stiffness. Recently, the authors have been applying a human amniotic membrane graft to the dorsal aspect of the first metatarsal head before closure of the first metatarsophalangeal joint capsule. The authors have found this to help reduce inflammation and adhesions associated with the surgery. Patients who receive the membrane on the dorsal first metatarsal head after distal metatarsal osteotomies generally have less pain and swelling, and a better range of first MPJ motion after surgery in comparison to control patients
Summary
An array of distal first metatarsal osteotomies has been described over the decades for the correction of hallux valgus. Many of these osteotomies have been discarded or modified throughout the years. No one procedure is proficient in correcting all forms and severities of hallux valgus deformities. To optimize results, it is imperative for the surgeon to match a procedure and its modifications to the patient’s deformity. The authors consider the dorsal long arm chevron osteotomy stands at the forefront for correction of mild to moderate hallux abductovalgus. The results with this specific osteotomy are predictable; it allows for early ambulation, and it is easily modified to compensate for the deformity at hand.
References 1. Austin DW, Leventen EO. A new osteotomy for hallux valgus: a horizontally directed “V” displacement osteotomy of the metatarsal head for hallux valgus and primus varus. Clin Orthop. 1981;157:25–302. Reverdin J. De la deviation en dehors du gros orl (hallux valgus) et son traitement chirurgical. Trans Int Med Congr. 1881;2:408–4123. Jenkin WM, Todd WF. Osteotomies of the first metatarsal head: reverdin, reverdin modifications, Hohmann, Hohmann modifications. In: Gerbert J editors. Textbook of bunion surgery. 2nd edition. Mt Kisco (NY): Futura; 1991;4. Laird PO, Silvers SH, Somdahl J. Two reverdin-laird osteotomy modifications for correction of hallux abducto valgus. J Am Podiatr Med Assoc. 1988;78:4035. Zyzda MJ, Hinesar W. Distal L osteotomy in treatment of hallux abducto valgus. J Foot Surg. 1989;28:4456. Lombardi CM, Silhanek AD, Connolly FG, et al. First metatarsocuneiform arthrodesis and Reverdin-Laird osteotomy for treatment of hallux valgus: an intermediate-term retrospective outcomes study. J Foot Ankle Surg. 2003;42:77–857. Warrick JP, Edelman R. The Hohmann bunionectomy utilizing A-O screw fixation: a preliminary report. J Foot Surg. 1984;23:268–2748. Hawkins FB, Mitchell CL, Hedrick DW. Correction of hallux valgus by metatarsal osteotomy. J Bone Joint Surg Am. 1945;27:3879. Merkel KD, Katoh Y, Johnson EW. Mitchell osteotomy for hallux valgus: long-term follow-up and gait analysis. Foot Ankle. 1983;3:189–19610. Helal B, Gupta SK, Gojosen P. Surgery for adolescent hallux valgus. Acta Orthop Scand. 1974;45:27111. Grace D, Hughes J, Klenerman L. A comparison of Wilson and Hohmann osteotomies in the treatment of hallux valgus. J Bone Joint Surg Br. 1988;70:236–24112. Allen TR, Gross M, Miller J, et al. The assessment of adolescent hallux valgus before and after first metatarsal osteotomy. Int Orthop. 1981;5:11113. Johnson JB, Smith SD. Preliminary report on derotational, angulational, transpositional osteotomy: a new approach to hallux abducto valgus surgery. J Am Podiatry Assoc. 1974;64:667–67514. Jahss MH, Troy AI, Kummer F. Roentgenographic and mathematical analysis of first metatarsal osteotomies for metatarsus primus varus: a comparative study. Foot Ankle. 1985;5:280–32115. Hattrup SJ, Johnson KA. Chevron osteotomy: analysis of factors in patients’ dissatisfaction. Foot Ankle. 1985;5:327–33216. Kalish SR. Modifications of the Austin hallux valgus repair (Kalish osteotomy). In: McGlamry ED editors. Reconstructive surgery of the foot and leg-update ’89. Tucker (GA): Podiatry Institute; 1989;p. 14–1917. Youngswick FD. Modifications of the Austin bunionectomy for treatment of metatarsus primus elevatus associated with hallux limitus. J Foot Surg. 1982;21(2):11418. Bösch P, Wanke S, Legenstein R. Hallux valgus correction by the method of Bösch: a new technique with a seven- to ten-year follow-up. Foot Ankle Clin. 2000;5:485–49819. Giannini S, Ceccarelli F, Bevoni R, et al. Hallux valgus surgery: the minimally invasive bunion correction (SERI). Tech Foot Ankle Surg. 2003;2:11–2020. Magnan B, Pezzè L, Rossi N, et al. Percutaneous distal metatarsal osteotomy for correction of hallux valgus. J Bone Joint Surg. 2005;87:1191–119921. Badway TM, Dutkowsky JP, Graves SC, et al. An anatomical basis for the degree of displacement of the distal chevron osteotomy in the treatment of hallux valgus. Foot Ankle. 1997;18(4):213–21522. Stienstra JJ, Lee JA, Nakadate DT. Large displacement distal chevron osteotomy for the correction of hallux valgus deformity. Foot Ankle. 2002;41:213–22023. Jones RO, Harkless LB, Baer MS, et al. Retrospective statistical analysis of factors influencing the formation of long-term complications following hallux abducto valgus surgery. J Foot Surg. 1991;30:344–34924. Jahss MH. Disorders of the hallux and the first ray, ch 39. In: Jahss MH editors. Disorders of the foot and ankle: medical and surgical management. 2nd edition. Philadelphia: WB Saunders Co; 1991;p. 943–117325. Shapiro F, Heller L. The Mitchell distal metatarsal osteotomy in the treatment of hallux valgus. Clin Orthop. 1975;107:225–23126. Hirvensalo E, Bostman O, Tormala P. Chevron osteotomy fixed with absorbable polyglycolide pins. Foot Ankle. 1991;11:212–21827. Jones KJ, Feiwell LA, Freedman EL. The effect of chevron osteotomy with lateral capsular release on the blood supply to the first metatarsal head. J Bone Joint Surg Am. 1995;77:197–204
 I have never been in the least bit disappointed in the results and kindness of Dr. Franson ans his staff during the approximate...Fred S.
I have never been in the least bit disappointed in the results and kindness of Dr. Franson ans his staff during the approximate...Fred S. Good diagnostics and explanation. Both Dr and staff meet my first 5 minute rule.Alvin L.
Good diagnostics and explanation. Both Dr and staff meet my first 5 minute rule.Alvin L. The very Best!Antoinette O.
The very Best!Antoinette O. Instant and energetic response is provided to any question or need that I might have. I have the highest confdcence in Dr. Bar...Michael M.
Instant and energetic response is provided to any question or need that I might have. I have the highest confdcence in Dr. Bar...Michael M. Very satisfiedJay G.
Very satisfiedJay G. Just Thank you! All is always the best services . Highly recommend.Ingrid F.
Just Thank you! All is always the best services . Highly recommend.Ingrid F. Excellent people. Excellent care.Bradley S.
Excellent people. Excellent care.Bradley S. The personal me trata con respeto mi doctor está tratando de que aser lo mejor para mi perdona graciasArmando T.
The personal me trata con respeto mi doctor está tratando de que aser lo mejor para mi perdona graciasArmando T. 100% satisfiedJames R.
100% satisfiedJames R. Hate these surveys.Rebecca A.
Hate these surveys.Rebecca A. Dr. Nalbandian provided a good understanding of my options and will follow up in 3 months to see how I am doing and what I shou...William B.
Dr. Nalbandian provided a good understanding of my options and will follow up in 3 months to see how I am doing and what I shou...William B. I just got back from playing tennis, my favorite activity and I have Dr. Baravarian to thank!
I just got back from playing tennis, my favorite activity and I have Dr. Baravarian to thank!
I have a long back story. I frac...Em M.
-
 Listen Now
Revealing the Secrets of Men's and Women's Shoe Sizes: Why Are They Different?
Read More
Listen Now
Revealing the Secrets of Men's and Women's Shoe Sizes: Why Are They Different?
Read More
-
 Listen Now
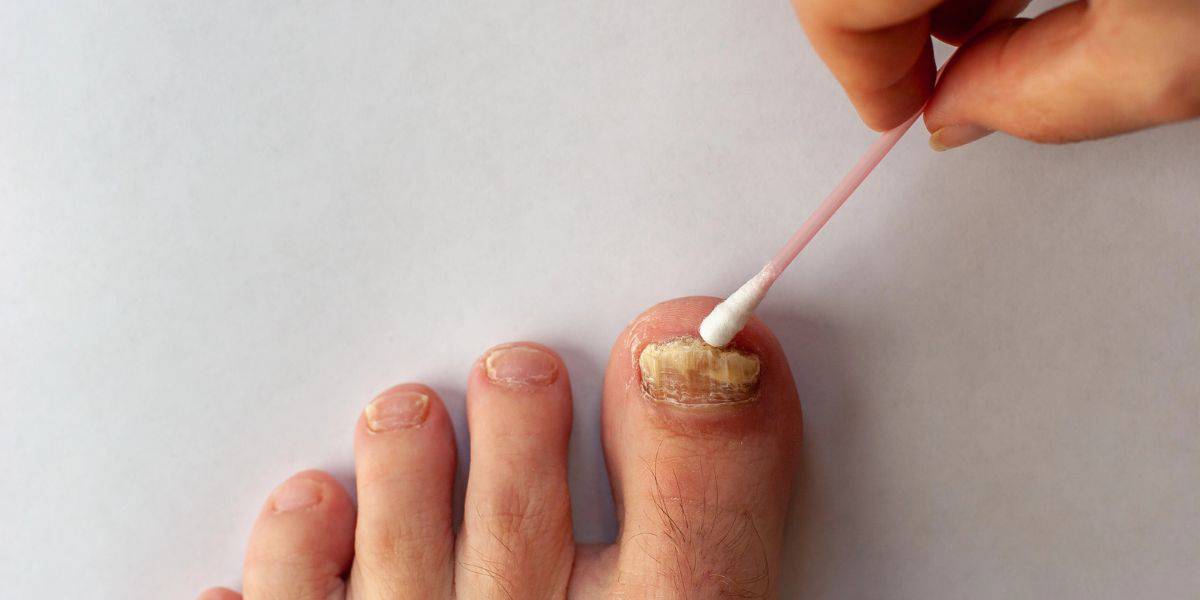
What To Do When Your Toenail Is Falling Off
Read More
Listen Now
What To Do When Your Toenail Is Falling Off
Read More
-
 Listen Now
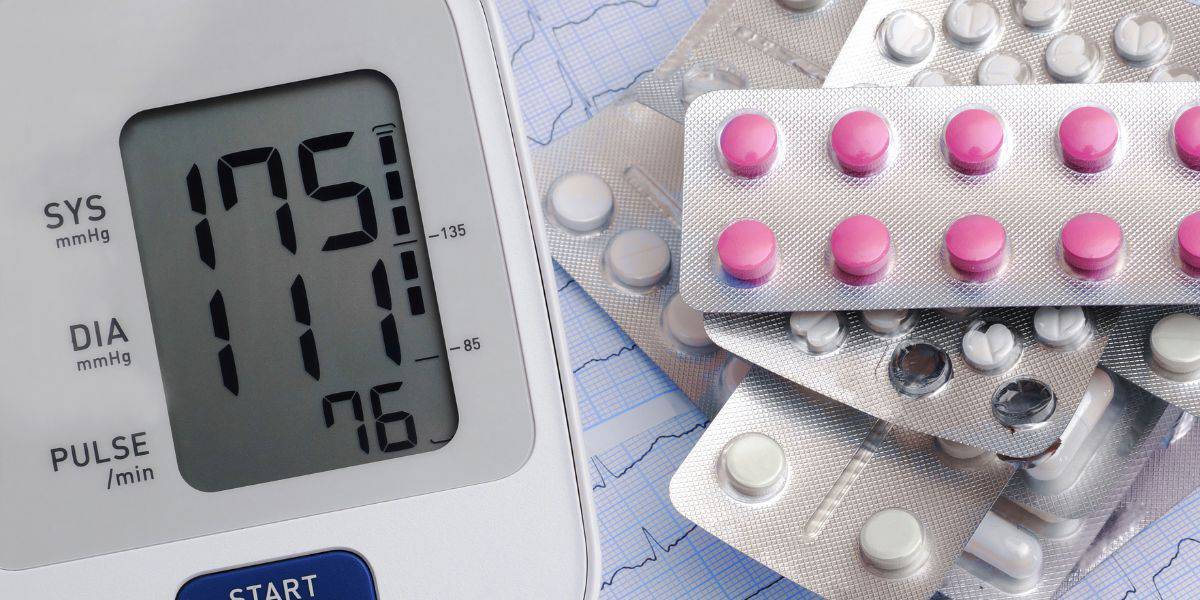
Do Blood Pressure Medicines Cause Foot Pain?
Read More
Listen Now
Do Blood Pressure Medicines Cause Foot Pain?
Read More
-
 Listen Now
15 Summer Foot Care Tips to Put Your Best Feet Forward
Read More
Listen Now
15 Summer Foot Care Tips to Put Your Best Feet Forward
Read More
-
 Listen Now
How To Tell If You Have Wide Feet
Read More
Listen Now
How To Tell If You Have Wide Feet
Read More
-
 Listen Now
How Many Steps Do I Need A Day?
Read More
Listen Now
How Many Steps Do I Need A Day?
Read More
-
 Listen Now
What Are Shin Splints?
Read More
Listen Now
What Are Shin Splints?
Read More
-
 Listen Now
Flip-flops Causing You Pain? Protect Your Feet This Summer!
Read More
Listen Now
Flip-flops Causing You Pain? Protect Your Feet This Summer!
Read More
-
 Listen Now
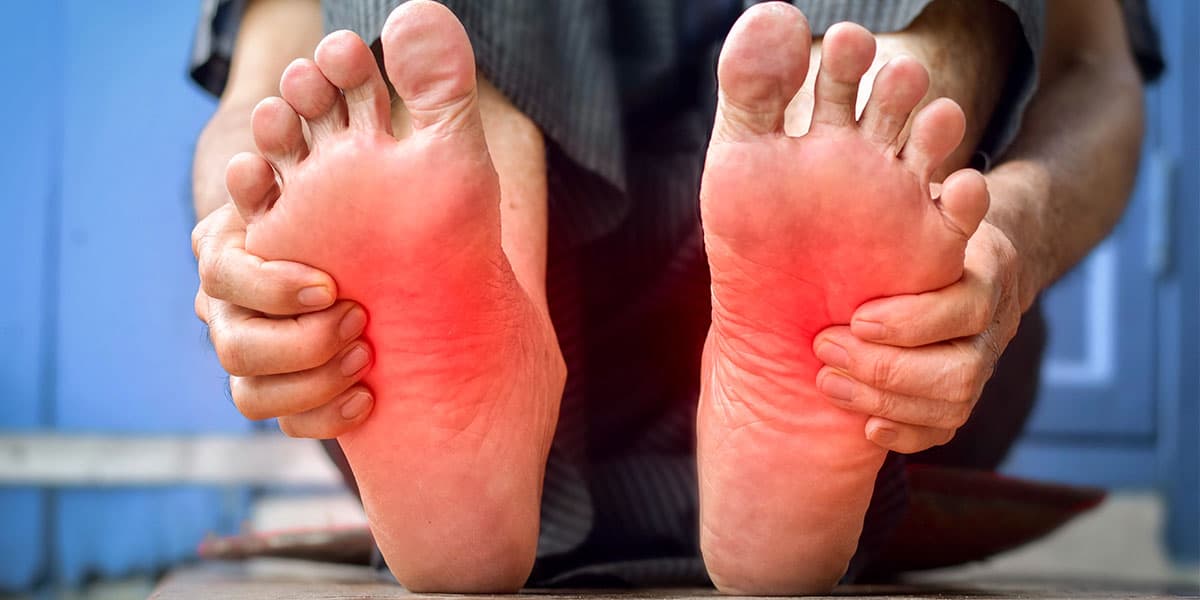
What Is Erythromelalgia?
Read More
Listen Now
What Is Erythromelalgia?
Read More
-
 Listen Now
Could Feet Be the Windows to Your Health?
Read More
Listen Now
Could Feet Be the Windows to Your Health?
Read More
-
 Listen Now
Why Are My Feet Different Sizes? It's More Common Than You Think
Read More
Listen Now
Why Are My Feet Different Sizes? It's More Common Than You Think
Read More
-
 Listen Now
Is Foot Analysis Better than Horoscopes? What Do Your Toes Reveal About Your Personality?
Read More
Listen Now
Is Foot Analysis Better than Horoscopes? What Do Your Toes Reveal About Your Personality?
Read More
-
 Listen Now
Custom Orthotics vs. Over-the-Counter Inserts: Which Are Best for Your Feet?
Read More
Listen Now
Custom Orthotics vs. Over-the-Counter Inserts: Which Are Best for Your Feet?
Read More
-
 Listen Now
Swollen Feet During Pregnancy
Read More
Listen Now
Swollen Feet During Pregnancy
Read More
-
 Listen Now
The Link Between Foot Health and Posture
Read More
Listen Now
The Link Between Foot Health and Posture
Read More














