- Home
- Advanced Treatments
- Wound Care Treatments
- Compression and Collagen Therapy for Wound Healing
Compression and Collagen Therapy for Wound Healing
Updated
3/7/2024
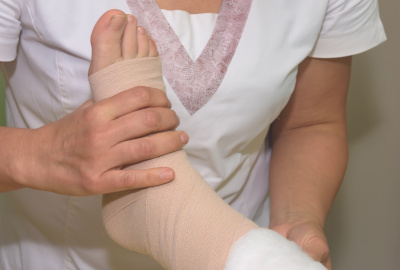
The wound experts at University Foot & Ankle Institute (UFAI) have a wealth of experience healing various types of wounds of the feet and legs — including diabetic foot ulcers, pressure ulcers, and venous leg ulcers (VLU).
Our podiatrists typically approach these chronic wounds with a combination of two therapies: a bilayered living cellular construct (BLCC) and an acellular fetal bovine collagen dressing (FBCD).
In simple terms, each therapy is a living cellular product, much like a bandage, and the key to each is collagen.
Related Content
19,681 Total 1st Party Reviews / 4.9 out of 5 Stars
 I went on a hiking trip in Seattle and got a wood sliver deep in my foot from a walk on the beach. After 2 weeks of event work ...Sandi P.
I went on a hiking trip in Seattle and got a wood sliver deep in my foot from a walk on the beach. After 2 weeks of event work ...Sandi P. Overall, it was a great experience. I've been coming to Dr. Kellman for about a year and he and his staff are very helpful.Vanessa W.
Overall, it was a great experience. I've been coming to Dr. Kellman for about a year and he and his staff are very helpful.Vanessa W. ExcellentDebasish M.
ExcellentDebasish M. Everyone was friendly and professional.Victor L.
Everyone was friendly and professional.Victor L. Dr Baravarian is awesome! I say this because he's perfectly willing to admit when he doesn't know something and when he cannot...Julie D.
Dr Baravarian is awesome! I say this because he's perfectly willing to admit when he doesn't know something and when he cannot...Julie D. Very efficient and an excellent serviceHorwitz J.
Very efficient and an excellent serviceHorwitz J. After suffering with a 20 year old ankle injury, I reluctantly agreed to consider PRP treatment. I was very skeptical that I co...Teresa C.
After suffering with a 20 year old ankle injury, I reluctantly agreed to consider PRP treatment. I was very skeptical that I co...Teresa C. Chaos in the office checkin. We weren’t forewarned about the iPad data collection. That made me late for a following appointmen...Carl C.
Chaos in the office checkin. We weren’t forewarned about the iPad data collection. That made me late for a following appointmen...Carl C. Dr Nalbandian is an exceptional doctor and person. The staff respectfully & compently delt with an issue I had regarding a prev...Karen M.
Dr Nalbandian is an exceptional doctor and person. The staff respectfully & compently delt with an issue I had regarding a prev...Karen M. Visiting the office is a pleasurable occurance.Thomas J.
Visiting the office is a pleasurable occurance.Thomas J. Dr Kelman and his staff are always wonderfully caring and respectful to my father who has Alzheimer's dementia.Erland E.
Dr Kelman and his staff are always wonderfully caring and respectful to my father who has Alzheimer's dementia.Erland E. Thank you for being there for your patients.Dieter B.
Thank you for being there for your patients.Dieter B.
-
 Listen Now
Common Foot Problems In Aging Feet: What To Watch Out For
Read More
Listen Now
Common Foot Problems In Aging Feet: What To Watch Out For
Read More
-
 Listen Now
Revolutionizing Extremity Imaging: UFAI's Open MRI for the Foot and Ankle
Read More
Listen Now
Revolutionizing Extremity Imaging: UFAI's Open MRI for the Foot and Ankle
Read More
-
 Listen Now
Why Are My Feet Different Sizes? It's More Common Than You Think
Read More
Listen Now
Why Are My Feet Different Sizes? It's More Common Than You Think
Read More
-
 State-of-the-Art CT Scanning, Now in Our Office
Read More
State-of-the-Art CT Scanning, Now in Our Office
Read More
-
 Listen Now
The Link Between Foot Health and Posture
Read More
Listen Now
The Link Between Foot Health and Posture
Read More
-
 Listen Now
Custom Orthotics vs. Over-the-Counter Inserts: Which Are Best for Your Feet?
Read More
Listen Now
Custom Orthotics vs. Over-the-Counter Inserts: Which Are Best for Your Feet?
Read More
-
 Listen Now
Revealing the Secrets of Men's and Women's Shoe Sizes: Why Are They Different?
Read More
Listen Now
Revealing the Secrets of Men's and Women's Shoe Sizes: Why Are They Different?
Read More
-
 Listen Now
Could Feet Be the Windows to Your Health?
Read More
Listen Now
Could Feet Be the Windows to Your Health?
Read More
-
 Listen Now
15 Summer Foot Care Tips to Put Your Best Feet Forward
Read More
Listen Now
15 Summer Foot Care Tips to Put Your Best Feet Forward
Read More
-
 Listen Now
Do blood pressure medicines cause foot pain?
Read More
Listen Now
Do blood pressure medicines cause foot pain?
Read More
-
 Listen Now
Is Foot Analysis Better than Horoscopes? What Do Your Toes Reveal About Your Personality?
Read More
Listen Now
Is Foot Analysis Better than Horoscopes? What Do Your Toes Reveal About Your Personality?
Read More
-
 Listen Now
How to Choose Running Shoes: 6 Essential Steps
Read More
Listen Now
How to Choose Running Shoes: 6 Essential Steps
Read More
-
 Listen Now
Flip-flops Causing You Pain? Protect Your Feet This Summer!
Read More
Listen Now
Flip-flops Causing You Pain? Protect Your Feet This Summer!
Read More
-
 Listen Now
9 Running Tips from Sports Medicine Experts
Read More
Listen Now
9 Running Tips from Sports Medicine Experts
Read More
-
 Listen Now
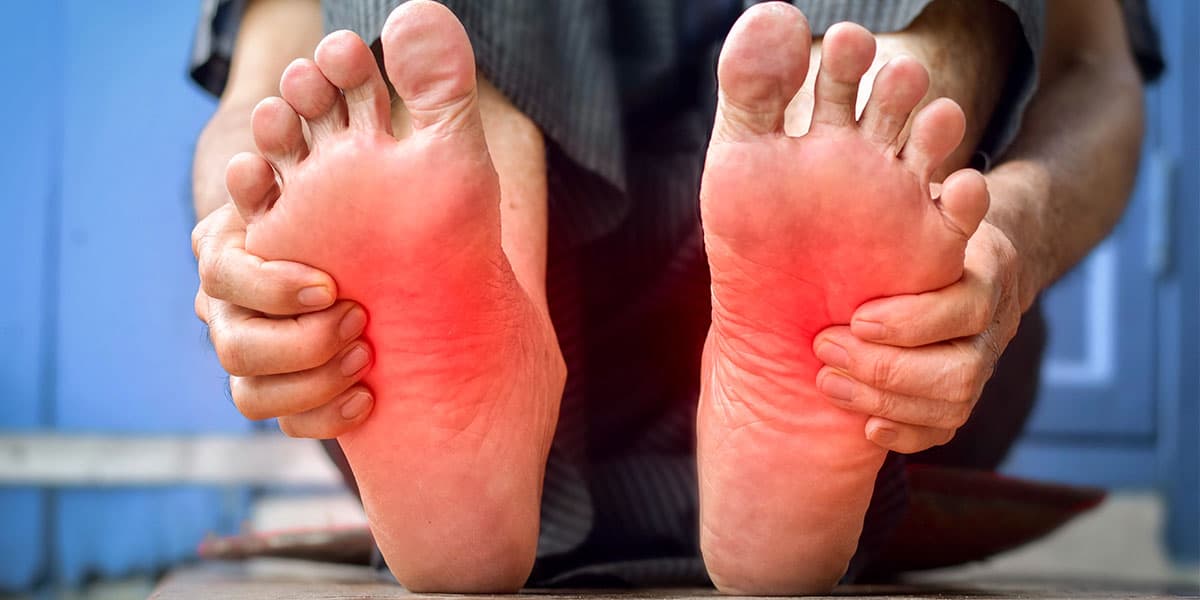
What is erythromelalgia?
Read More
Listen Now
What is erythromelalgia?
Read More














