- Home
- Foot & Ankle Conditions
- Arthritic Conditions
- Hallux Rigidus
Arthritic Conditions: Big Toe Arthritis (Hallux Rigidus)
Updated
12/1/2023
In this video, we discuss Big Toe Arthritis and the advanced treatment options available at UFAI.
What's hallux rigidus?
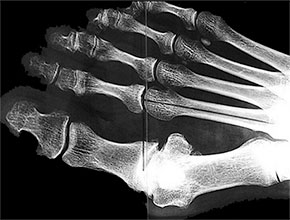
Also known as big toe arthritis, hallux rigidus is a form of degenerative arthritis that affects the joint at the base of the big toe.
This condition often leads to stiffness, swelling, and pain in the affected joint, particularly during activities that require bending of the toe
Table of Contents
- Hallux limitus vs. hallux rigidus: what's the difference?
- What are the symptoms of hallux rigidus and hallux limitus?
- What are causes and risk factors of hallux limitus and hallux rigidus?
- How is hallux limitus and hallux rigidus diagnosed?
- Non-surgical treatments for hallux rigidus
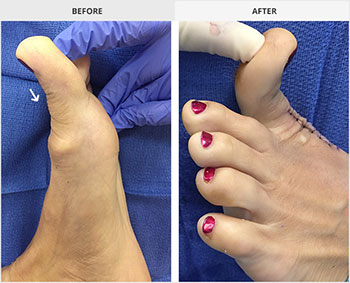
- Surgical options for hallux rigidus
- UFAI offers the most advanced treatment for big toe joint pain and hallux rigidus
- Frequently Asked Questions about Hallux Limitus
- Can hallux rigidus cause knee or back pain?
- Can hallux rigidus cause other problems?
- Can hallux rigidus cause plantar fasciitis?
- Can you run with hallux rigidus?
- How to prevent hallux rigidus?
- What are the best shoes for hallux rigidus?
- Will orthotics help big toe arthritis?
- Do you use the Hemi joint implant for hallux ridigus treatment?
Related Content
19,485 Total 1st Party Reviews / 4.9 out of 5 Stars
 Polite staff; great patient "connection".Warren M.
Polite staff; great patient "connection".Warren M. Great experience. Great communication. Great direction for my care. Very happy I chose to go with this particular doctor and o...Christopher R.
Great experience. Great communication. Great direction for my care. Very happy I chose to go with this particular doctor and o...Christopher R. Great service and care. Highly recommend Dr. Franson.David B.
Great service and care. Highly recommend Dr. Franson.David B. If you have to go see a Doctor than this is a great experience.Frank M.
If you have to go see a Doctor than this is a great experience.Frank M. My doctor was great. Really greatRudolph B.
My doctor was great. Really greatRudolph B. Good.David E.
Good.David E. I highly recommend Dr. Bob Baravarian, DPM of UFAI. He and a team of other professionals spent time to identify the issue and p...Michael K.
I highly recommend Dr. Bob Baravarian, DPM of UFAI. He and a team of other professionals spent time to identify the issue and p...Michael K. Your Santa Barbara office and Dr. Johnson always give me excellent care!Jayne A.
Your Santa Barbara office and Dr. Johnson always give me excellent care!Jayne A. Dr Bob is the best! Very conservative and makes sure all options done before jumping into a surgery....Jennifer S.
Dr Bob is the best! Very conservative and makes sure all options done before jumping into a surgery....Jennifer S. Dr. Gina Nalbadian was amazing!! I came in with an emergency foot situation and she had wonderful bedside manner and resolved m...Danielle C.
Dr. Gina Nalbadian was amazing!! I came in with an emergency foot situation and she had wonderful bedside manner and resolved m...Danielle C. I was frustrated that after 3 weeks I still hadn’t heard back about my PT referral status. And I did sit in a room for over 30 ...Sarah C.
I was frustrated that after 3 weeks I still hadn’t heard back about my PT referral status. And I did sit in a room for over 30 ...Sarah C. I’m very pleased with Dr. Kelman.Alan S.
I’m very pleased with Dr. Kelman.Alan S.
-
 Listen Now
Revolutionizing Extremity Imaging: UFAI's Open MRI for the Foot and Ankle
Read More
Listen Now
Revolutionizing Extremity Imaging: UFAI's Open MRI for the Foot and Ankle
Read More
-
 Listen Now
Is Barefoot Running Better? Or are you Running Toward Injury?
Read More
Listen Now
Is Barefoot Running Better? Or are you Running Toward Injury?
Read More
-
 StimRouter: A Revolutionary Approach to Targeted Pain Relief
Read More
StimRouter: A Revolutionary Approach to Targeted Pain Relief
Read More
-
 Listen Now
Flip-flops Causing You Pain? Protect Your Feet This Summer!
Read More
Listen Now
Flip-flops Causing You Pain? Protect Your Feet This Summer!
Read More
-
 Listen Now
9 Running Tips from Sports Medicine Experts
Read More
Listen Now
9 Running Tips from Sports Medicine Experts
Read More
-
 Listen Now
Common Foot Problems In Aging Feet: What To Watch Out For
Read More
Listen Now
Common Foot Problems In Aging Feet: What To Watch Out For
Read More
-
 Listen Now
If the Shoe Fits, Wear it… Especially for Kids Shoes!
Read More
Listen Now
If the Shoe Fits, Wear it… Especially for Kids Shoes!
Read More
-
 Listen Now
The Power of Pediatric Flexible Flatfoot Procedures
Read More
Listen Now
The Power of Pediatric Flexible Flatfoot Procedures
Read More
-
 Listen Now
Custom Orthotics vs. Over-the-Counter Inserts: Which Are Best for Your Feet?
Read More
Listen Now
Custom Orthotics vs. Over-the-Counter Inserts: Which Are Best for Your Feet?
Read More
-
 Listen Now
Revealing the Secrets of Men's and Women's Shoe Sizes: Why Are They Different?
Read More
Listen Now
Revealing the Secrets of Men's and Women's Shoe Sizes: Why Are They Different?
Read More
-
 Listen Now
Why Are My Feet Different Sizes? It's More Common Than You Think
Read More
Listen Now
Why Are My Feet Different Sizes? It's More Common Than You Think
Read More
-
 Listen Now
The Link Between Foot Health and Posture
Read More
Listen Now
The Link Between Foot Health and Posture
Read More
-
 Listen Now
An Inside Look at Shockwave Therapy for Heel Pain, now available in Valencia, CA
Read More
Listen Now
An Inside Look at Shockwave Therapy for Heel Pain, now available in Valencia, CA
Read More
-
 Listen Now
How to Choose Running Shoes: 6 Essential Steps
Read More
Listen Now
How to Choose Running Shoes: 6 Essential Steps
Read More
-
 State-of-the-Art CT Scanning, Now in Our Office
Read More
State-of-the-Art CT Scanning, Now in Our Office
Read More